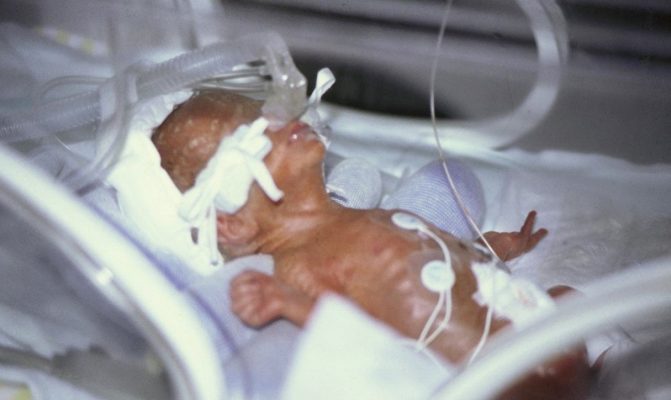
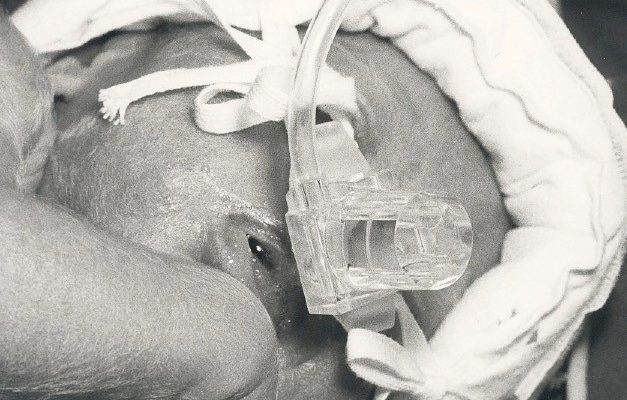
After spending endless nights making prototypes in a basement, doctors Kjell Nilsson and Gunnar Moa finally solved the riddle on how to help prematurely born babies breathe. Over 30 years later, their innovation has saved the lives of thousands of children all around the world – and still continues to do so.
Struggling to cope
Kjell Nilsson remembers his first encounter with prematurely born babies who were struggling to breathe on their own. He was working as an anaesthetic doctor at a provincial hospital in Östersund, northern Sweden, where the intensive care and anaesthetics units operated as one.
“The babies often needed a respirator, a breathing machine. We had to sit there all throughout the night and frequently adjust the machine to make sure they even survived.”
At the time, the breathing support CPAP (Continuous Positive Airway Pressure) was put over the babies’ heads to help them breathe. The system created a distending pressure in their lungs, resulting in improved ventilation. In the 1980s, the existing CPAP solutions were however technically flawed and proved a great strain for the prematurely born babies who were already struggling.
“Many of these babies couldn’t cope for more than 24 hours with the old CPAP technique as the breathing resistance was often too high. Due to the shortcomings of the CPAP systems they often ended up being sent to intensive care where they were hooked up to a respirator.”
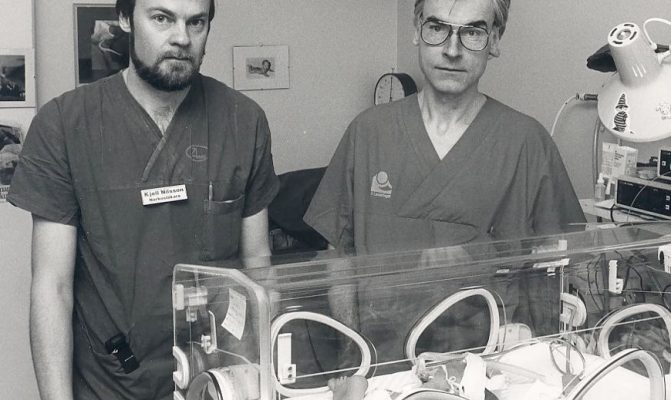
“My colleague Gunnar and I agreed that it shouldn’t have to be like this. There just had to be a better technical solution to the CPAP-treatment.”
Head-wind to get ahead
The two doctors came up with some ideas on how they might be able to solve the problem. After long days working at the Östersund hospital, Kjell and Gunnar spent their evenings and nights in Kjell’s workshop trying to think of an alternative solution to help the children.
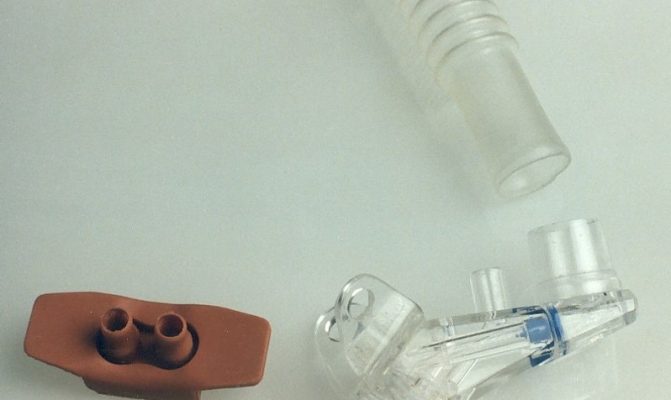
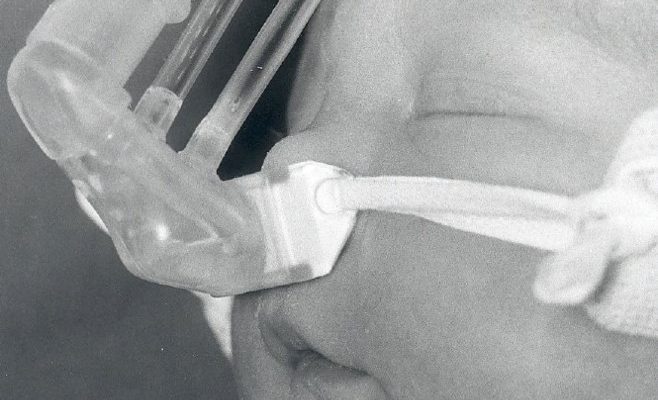
What they came up with was a ground-breaking innovation. The concept was a unique nasal prong with an integrated flow/pressure generator from which the baby receives an oxygen/air mixture. Its flow determines the airway pressure in the baby’s lungs – one could say it generates a head-wind into the baby’s nose. How much head-wind the baby receives is decided by how inflated the lungs should be. Once the lungs get inflated, they become more elastic, which makes it easier for the baby to breathe. In addition, the oxygenating increases.
“If you have ever stood in strong head-wind and opened your mouth, you might have felt how your lungs expand. This is the same principle,” says Kjell.
One of the first to try it out
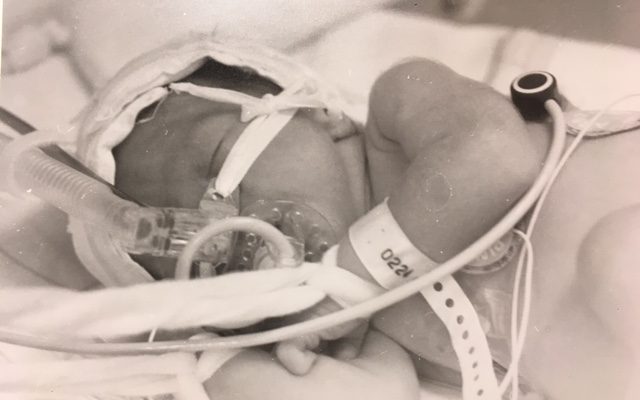
The doctors started to use their innovation to help the prematurely born babies at Östersund hospital in the late 80s. One of the first babies to receive the new breathing aid was Laila Majiet’s daughter Sandra in 1988. After Laila had contracted a severe case of preeclampsia, Sandra was born with underdeveloped lungs in week 34.
“You could see on her tiny chest she was struggling to breathe,” remembers mother Laila.
The parents were asked if they wanted to try the new breathing aid by Sandra’s physician – Gunnar Moa. They gladly accepted the offer. Sandra was placed in an incubator and received oxygen via the new system. A week later, she was able to breathe without assistance.
“I am happy and grateful that this breathing aid was available,” says Laila.
“They told me that the survival rate for premature babies at Östersund hospital at the time was unusually high. It might have been a result of the new CPAP system.”
It was clear that Kjell and Gunnar were onto something. After applying for a patent to protect and license their innovation, the next step was to find a manufacturer. The duo found the right match in a small British company called EME, which started to manufacture and sell the Swedish CPAP system.
“We had previously presented our innovation for several larger manufacturers in MedTech, but they couldn’t see the need or the market for it, says Kjell.
“As we did not have the means to manufacture the CPAP ourselves, it was crucial that we had a patent in place in order to license the innovation.”
New innovations
Although he has been in the business for over 30 years, Kjell is still looking for new and unique ways of improving neonatal care technology. In 2008 he started a new research project together with a colleague at Östersund hospital, Thomas Drevhammar. The aim of the project was to create new tools for respiratory support that can be used to avoid intubation and mechanical ventilation on premature infants. The research has been a collaboration between Östersund hospital and Karolinska Institutet. The group is growing and has led to one dissertation and two more PhD students.
The team’s latest innovation is an extension of the original CPAP system but which allows manual ventilation of new-born infants who do not breathe.
“The babies who are born very early sometimes need artificial breathing assistance for a minute or two before they can breathe on their own. Previously, you had to disconnect the CPAP, put a mask over the baby’s nose and mouth and squeeze a bag to help the baby breathe. It is crucial to have the CPAP at the resuscitation table in the delivery room. You can prevent the babies’ lung capacity from deteriorating and increase their odds of surviving if you treat them with CPAP as soon as possible,” explains Kjell.
“We realised that if we already have a CPAP system in place, which the baby will use during its first days, it can also be used during resuscitation to ensure a controlled amount of airway pressure is administered without risking any damage.”
Patent is key
Patenting and licensing their innovation has been key to Neores’s success. It is very difficult to move to production and CE-marking without acceptable IP protection. Kjell and Thomas chose to change IP service provider from a Stockholm-based firm to Awapatent and Patent Consultant Steve Athle, as they offered local expertise and personal meetings in Östersund.
“Steve was quick to understand what was important to cover in a patent application. Since our first meeting, Awapatent has been managing all our Intellectual Property.”
In addition to the method of resuscitation, the team has applied for a patent for an innovation which entails administering medicine to prematurely born babies through a breathable aerosol while using the CPAP.
“It is like an asthma medicine. You inhale it. It’s a mist with tiny drops consisting of the medicine. It is a gentler method on the child and easier to administer.”
Kjell and Thomas combine research grants to fund basic research with private investments for patents. There is a strong link between basic research, prototype production and ideas that can result in clinical products. Key to quick production has also been to use new technology, such as CAD/CAM software and 3D printers. Kjell was able to manufacture affordable prototypes for the resuscitation system and go from idea or revision to tests in a flow simulation laboratory.
“This was much more time consuming 30 years ago when every modification needed days or weeks of complex manufacturing.”
Across the world
Kjell and Gunnar’s original CPAP design is still used today. It has become the standard treatment system for prematurely born babies struggling to breathe all over the world. The invention has probably helped thousands of infants to survive and prevented disability from lung disease.
“It is an amazing feeling knowing that this system, which we came up with 30 years ago down in my basement in Östersund, has made a true difference, says Kjell.
“The fact that we chose to license our patent meant that the CPAP innovation could really take off. Gunnar and I would never have been able to manufacture it nor would we had a clue on how to sell it on the global market.”
The new company Neores, founded by Thomas and Kjell, has chosen a similar approach to IP and licensing.
“To acquire IP protection and license manufacturing and sales is the only way research and development in small companies can get products to a global market”, says Kjell.
“This way, we can continue to make a difference to prematurely born babies across the world.”